Different Restorative Systems In Non Carious Cervical Lesions
Özge Türkoğlu 1, Serdar Bağlar 2, Ali Can Bulut 3*
1 Oral Health Center of Kırıkkale, Turkey Republic Ministry of Health, Turkey.
2 Department of Restorative Dentistry, Faculty of Dentistry, University of Kırıkkale, Kırıkkale, Turkey.
3 Department of Prosthodontics, Faculty of Dentistry, University of Kırıkkale, Kırıkkale, Turkey.
|
|
Introduction
Oral health is integral to general well-being 1, 2 and relates to the quality of life 3, 4. The most common reason for tooth and dental hard tissue loss is dental caries. One of the common problems associated with dental hard tissue loss is tooth wear. Tooth wear is the reason for the irreversible loss of dental hard tissue in the absence of dental caries.5 It can manifest as abrasion, attrition, abfraction and erosion.6 Tooth wear has multiple etiologies.7 Tooth wear causes cavities with or without pain on occlusal and cervical areas. Tooth wear on the cervical area is named as ‘Non-Carious Cervical Lesions (NCCLs)’. NCCLs develop as a result of erosion, abrasion, and abfraction. NCCLs are characterized by the loss of dental hard tissue at the cementoenamel junction in the absence of caries. NCCLs margins include enamel, dentin, and cement.8-10
The prevalence of NCCLs has been estimated to vary between 5% and 85% of the population. NCCLs have a strong tendency to increase with age. They are very common at middle-aged and elderly individuals and represent a challenge to the dental profession.11 NCCLs can cause tooth sensitivity, pulp damage, and plaque retention due to cavitation.12 The decision for restorative procedures should be based on careful consideration of etiology and complex morphology. In restorative procedures of NCCLs, one of the difficulties is bonding to sclerotic dentin; another one is the isolation at the cervical area because the NCCLs are very close to periodontal tissues.
Clinicians have tried many restorative materials and techniques to obtain the best performance for NCCLs’ restorative treatments.13, 14 There are no bonding application strategy or restorative material systematically recognized as the ideal restorative systems for noncarious cervical lesions’ restorative treatment in the literature. When choosing a restorative system for NCCLs, we need to consider esthetic demands, longevity, durability, and marginal sealing ability as the major priorities. Packable and flowable compomers, giomers, and resin-based composites have been used for class V restorations and also NCCLs restorative treatments. All these materials have satisfactory esthetic properties and high wear resistance.
A major problem with restorative dentistry is the replacement of restorations because of secondary caries.15 Fluoride is effective in secondary caries prevention. The restorative materials that release fluoride can be advantageous. packable and flowable compomers and giomers are used because they release fluoride. Compomers combine glass ionomer cement and resin composites. Fluoride is released from aluminosilicate glass filler.16
Recently developed technologies as a new class of material fluoride-releasing and recharging giomers have been released to the market. The name "Giomer" is a mixture of the words ‘glass ionomer’ and ‘composite’. Giomers are based on PRG (pre-reacted glass ionomer) technology, in which a pre-reacted glass ionomer cement is used as filler.17
Giomers are different from compomers and resin-based composites. Resin-based composites do not release fluoride. The amount of fluoride release from giomers is more than compomers. In compomers, no silica-aluminosilicate glass particle reactions occur and no fluoride release is valid until water is absorbed by compomer. Fluoride recharge takes place in giomers but not in compomers. Compared with compomers, giomers have a stable glass ionomer phase and they can recharge fluoride. The hydrogel layer of giomers is thicker than compomers because in giomers the reactive fluoro-aluminosilicate glass and polyacid are added to the resin as components.18-20
Although it is not clearly understood how the fluoride is being recharged, it is being considered that the hydrogel layer is an effective factor. Fluoride recharge in giomers can be obtained from toothpaste, mouth rinses, or topical fluoride applications.18
The performance of giomer, which is a new restorative material, has been tested several times in in-vitro studies but the effects in class V NCCLs clinical studies haven’t been reported.
The purpose of this one-blind clinical study was to evaluate and compare the clinical performance of packable and flowable composites, compomers and giomers systems for restoring Class V at NCCLs, by using a modified/USPHS criteria in categories retention, color match, marginal discoloration, marginal adaptation, secondary caries, surface texture and anatomic form for 12 months (at 5% significant level).
The null hypothesis was that six different restorative systems performed equally regarding clinical quality and survival for 12 months.
Materials and Methods
This one-blind clinical study lasted 12 months, during which the clinical evaluation of the treatment of NCCLs with six different tooth-colored materials was carried out. The study included 33 patients (15 female, 18 male), aged between 35 and 85 years.
The cases included in this study were selected from the dental clinic of Kırıkkale University School of Dentistry, Department of Conservative Dentistry. The protocol of this study and written consent of the cases were reviewed and approved by the Kırıkkale University Ethics Committee on Investigations Involving Human Subjects. Written informed consent was obtained from all participants before treatment.
The criteria that are required for the volunteers to be accepted to the research are as follows: The volunteer has to be over 18 years, willing to be involved in the study, aware of the content of the study, accept to come to routine controls once per three months. In each quarter jaw, there have to be at least two NCCLs in vital permanent teeth and absence of periodontitis and periradicular lesions, traumatic occlusion, bruxism, and wear facets.
The criteria for excluding patients from the study were pulp pathology of teeth, diagnosed caries with cervical defects, and patients with mobile or fixed prosthetic restorations in the immediate environment of the tooth restorations to be observed in the study.
In the radiology clinic of Kırıkkale University School of Dentistry, we have diagnosed 300 NCCLs cases in 33 patients (at least 8 in each) regardless of etiology.
In diagnoses, it is been attended that the size of the lesion would not be over 1/3 of the crown length of the tooth. No width and depth measurements were made in the lesions included in the study. In the study, the common properties of the lesions are that: the occlusal margins of the lesions are at the enamel tissues and occlusal margin, and the gingival margins of the lesions are at the dentine tissues. None of the lesions have reached the pulp. 188 of the NCCLs were posterior (molar and premolar), 112 of them were anterior (incisor and canine). All of the teeth that have been restored are normal occlusions and they all have antagonists against them.
Operative Procedures
300 NCCLs divided into six randomized groups (n=50). All of the lesions were cleaned with plain pumice in a rubber prophylaxis cup and rinsed with water. After shade selection, isolation was accomplished using cotton rolls and a saliva ejector, with no mechanical preparation or beveling.
Six different restorative systems were numbered from 1 to 6 that was used in the study randomized draws (Tablo 1). The restorative systems were defined as follows; group 1: FL-BondII and Beautiful II (FLB&B), group 2: FL-BondII and Beautiful Flow Plus F00 (FLB&BF), group 3: Prime Bond NT and Dyract XP (PBNT&DyXP), group 4: Prime Bond NT and Dyract Flowable (PBNT&DyF), group 5: Single Bond Universal and Filtek Ultimate (SBU&FU), group 6: Single Bond Universal and Filtek Ultimate Flow (SBU&FUF). The study used the following materials and adhesive systems shown in Table 2. All restorations were placed by one operator. The application of the restorative systems was determined as right upper, left upper, left lower, and right lower jaws. The study started from a lesion in the posterior lesion in the right upper jaw of the first patient. The restorative systems were applied to the patients in groups 1 to 6 respectively following the proposals of the manufacturers (Table 3).
Clinical evaluation
The first evaluation was made in the 1 week after placement and others 3rd, 6th, 9th, and 12th months respectively. The clinical quality of the restorations in this study was evaluated according to the Modified United States Public Health Service criteria (Table 4) by two independent examiners using a mirror and probe. A forced-consensus model was used to determine a final rating when there was disagreement between examiners.
Statistical Evaluation
The survival rate was analyzed with the Kaplan-Meier estimator and Log-Rank test; other criteria were analyzed among the groups with the Kruskal Wallis test. The cumulative survival rates of restorations over one year are shown in Figure 1. In all statistical tests were evaluated at 5% significant level via SSPS computer program (SPSS Ver. 20.0, SPSS Inc., Chicago, IL, USA).
Results
During the research process, a total of 300 NCCLs in 33 patients were evaluated with a 100% recall rate.
The percentage of survival rates is shown in Table 5. Statistically significant differences were found between the survival rates of restorations at the end of the 12-month evaluation period (p<0.05).
Survival rates were found statistically different between PBNT&DyXP and SBU&FU (p=0.016). The Log-Rank test indicated statistically significant differences among the survival rates of FLB&B and other groups (p<0.05), FLB&BF, and other groups (p<0.05).
No restorations in any group exhibited secondary caries at any evaluation period within this study. All of the restorations received ‘Alpha’ ratings in the final evaluation for secondary caries.
The percentage of alpha ratings for surface textures, anatomic forms, marginal adaptations, marginal discolorations, color matches decreased in time. At the end of the 12 months, percentage of ‘Alpha’ ratings for surface textures were higher than 90%, anatomic forms were higher than 95%, color matches were between 88-98%, marginal discolorations were between 83-97%, marginal adaptations were higher than 90% at all groups (Figure 2-5). For these criteria, no significant differences were found among groups by the Kruskal Wallis test (p>0.05).
At the end of 12 months, even there were no significant differences in terms of surface texture, anatomic form, marginal adaptation, marginal discoloration, color match among groups. PBNT&DyF group had demonstrated much more ‘Bravo’ rating in surface texture, marginal discoloration, color match criteria than other groups.
Discussion
Multiple etiologies, pathogenesis, diagnosis, complex morphology, and selection of restorative procedures for NCCLs represent a huge problem in dentistry. Although there are several studies in the literature for NCCLs, there are still many doubts and contradictions. NCCLs represent a big challenge for clinicians because of the difficulties in their restoration.21 Although there is a large number in vitro studies of developing restorative materials with the physical-mechanical properties, the results of in vitro studies can not be fully reflected in the behavior of materials in the oral environment. To assess the success of restorative materials which is included in the new material such as giomers, recent and actual clinical studies are needed.22, 23
In this study assessment rate is 100%. At many clinical studies,’ the most emphasized topic is longevity and durability of the restoration in the oral cavity. The retention of restorations is the key criterion by which the clinical efficiency of restorative materials is evaluated.
In this study, the retention rate at 3rd month of restorations were found 70% for FLB & B, 72% for FLB & BF, 96% for PBNT & DyXP, 100% for PBNT & DyF, 98% for SBU & FU 100% for SBU & FUF. Giomer ( FLB&B) and flowable giomer restorative systems (FLB & BF) that carry the quality of fluoride charge and recharge show more than 30% retention loss in the first 3 months. According to this result, choosing giomer and flowable giomer restorative systems for NCCLs’ restorative treatments should be considered twice before the application.
The retention rate at 6th month of restorations was found 68% for FLB & B, 70% for FLB & BF, 88% for PBNT & DyXP, 96% for PBNT&DyF, 98% for SBU&FU 100% for SBU&FUF. Most of the restorations were lost in the first six months. In the literature, a majority of losses of restorations have been reported in the early period. The key factor in the clinical studies evaluating the success of restorations that were applied to noncarious cervical lesions restoration is retention.24 The most retention loss in the compomer group (PBNT & DyXP) was observed in the first 6 months. At the end of this study, the difference in the retention rate between compomer and composite groups was found statistically/significantly different. When composite and compomer groups compared in retention, we can say that composite systems had higher survival rates than compomer systems.
24 months-long study by Stojanac et al. shows that there was a 20% retention loss in composite (Esthet.X/Prime & BondNT) and 16.7% in compomer (Dyract eXtra/Xeno III) restorations.23
Pollington & Van Noort R found retention rates of 86.6% for composite, and 86.7% for compomer after 36 months while using composite and compomer in combination with a self-etching adhesive system placed on NCCLs.25
The compomer restoration (for Dyract) retention rate was found 97% in a study done by Tyas (1998) at one year, 90% at three years in a study done by Folwaczny et al [2001a], 80% at five years in a study by Folwaczny et al [2001b].26-28
In our study 12th month retention rates were found 68% for FLB & B, 68% for FLB & BF, 84% for PBNT & DyXP, 96% for PBNT & DyF, 98% for SBU& FU, 94% for SBU & FUF. Retention rates were found statistically/significantly different between FLB & B and other groups; and between FLB & BF and other groups.
Determination of performance of restorations according to ADA (American Dental Association) criteria is as follows: up to 5% retention loss in two years, and 10% retention loss after four years is determined as clinically successful for restorative materials.14 According to the results of our 12-month clinical study by using ADA’s criteria, while FLB & B, FLB & BF, and PBNT & DyXP restorations were found unsuccessful, SBU& FU, SBU & FUF, and PBNT & DyF restorations were found successful in terms of retention.
It is hard to compare the durability and longevity of the restoration at NCCLs with other clinical studies since many factors affect the retention of restorations. The differences in the obtained results can be attributed to differences in the morphology of the cavity, variability, amount of sclerotic dentin, no mechanical retention cavity model, operator skills; type of occlusion; stress that causes a cervical region of the occlusal forces; difficulty in isolation; an oily layer that can leak from the air-water spray; surface preparation techniques (etching applications); binding capacity of the restorative system and the polymerization of the restorative materials.29, 30
Burrow and Tyas tested all-in-one adhesive in combination with the composite material for restoring NCCLs.31 They found retention rate was 100% at the end of the first year. A Huge deviation from the results of a similar clinical study by Brackett ve et al was observed.32 At the same combination, the retention rate was found 65% after a year. These studies show that it is hard to compare the restoration retention rate at NCCLs. There are no used systematically strategy bonding applications or recognized as the ideal restorative systems for noncarious cervical lesions restorative treatment in the literature.
The retention rate of the restoration at NCCLs can be related to the binding capacity of the restorative system. FLB&B and FLB & BF groups were applied self etch adhesive without additional use of acid etching. The loss of retention rate in the self etch adhesive groups (FLB & B and FLB & BF) was greater than the other groups in which acid etching was applied to the cavity surface. Too much loss of restoration at self etch groups may be associated with sclerotic dentin and self-etch adhesive system. It has been reported in the literature that total-etch and self-etch adhesive applications have different effects on the binding to sclerotic dentin. In vitro studies show that self-etching systems show less bond strength on sclerotic dentin compared to normal dentin.
In one study, show that the clinical performance of class V restorations is significantly influenced by the type of adhesive system. Etch & rinse systems should be chosen as self-etching systems.33 The dentin and enamel surfaces should be roughened before the placement of the restoration. It has been shown that the additional use of acid etching improves the clinical success of restorative materials at NCCLs in some studies.34
In an attempt to maximize the retention rates of restorations class V at NCCLs, low elastic-modulus materials are recommended. There were no significant differences found in retention rates between FLB & B and FLB & BF; and between SBU&FU and SBU & FUF. Flowable restorations which have a high modulus of elasticity showed no significant differences compared to packable restoration in retention rates. On the other hand, there was a significant difference in retention rates between PBNT & DyXP and PBNT & DyF. Compomer restorations showed a significantly lower retention rate than flowable compomers. We may prefer flowable compomer restorations instead of packable types in terms of longevity and durability in the restorative treatment of NCCLs according to this study findings.
Heymann et. Al 35 found the retention rates for restorations with a lower elastic modulus to be significantly higher than materials with higher elastic modulus. While in our study giomer and composite content groups don’t support this finding, compomer content groups do support it.
In a study done by Karaman et al.34 no significant difference was observed between the clinical performance of nanohybrid and flowable composite resins used in the restoration of NCCLs. This study shows that the high modulus of elasticity and also, the flexibility of the materials is not the only factor that affects retention rates, other factors also play a role.
At the end of this study, there was no statistically significant difference among groups for color match, retention, marginal discoloration, secondary caries, anatomic form, and marginal adaptation categories.
The loss of marginal adaptation is one of the most important factors that show the failure of restoration and the reason for replacement.36 Decline in rating (Alpha to Bravo) of marginal integrity on the large number of restorations at NCCLs is due to the small fracture of the cavo-surface margin caused by stress from polymerization shrinkage. Despite the improved bond strength of the materials, increased tooth flexure may still contribute to localized defects in marginal integrity for all materials.
A study by Onal and Pamir 37 demonstrated that more than two years of results could provide some information about the clinical performance of restorative materials. Two years is too short for the development of secondary caries. In this study, at the end of 12 months, no caries were found adjacent to the restorations, which is similar to several other clinical studies.
Conclusion
In literature, the majority of restoration loss has been reported in the early period. Most of the giomer (FLB&B), flowable giomer (FLB&BF), and compomer (PBNT &DyXP) restorations were lost in the first six months.
Although giomer, flowable giomer, and compomer restorations showed similar clinical qualities with other groups at other categories; they performed statistically significant less survival than other groups. They have shown insufficient clinical survival rates according to ADA acceptance guidelines.
After 12 months, flowable compomer (PBNT&DyF), composite (SBU& FU) and flowable composite (SBU&FUF) restorations have shown sufficient clinical survival, by terms of ADA acceptance guidelines.
The essence of this study was to show that nano-composite (SingBond Universal &Filtek Ultimate) restorations demonstrated better retention rates and clinical performances than other groups for all categories.
None of the restorations received a ‘Charlie’ rating in color match, marginal discoloration, secondary caries, anatomic form, and marginal adaptation categories but further evaluation is necessary for the measure means of long term clinical performances of these materials at NCCLs.
Statement of Ethics:
All procedures used were following the guidelines of the Helsinki Declaration on Human Experimentation.
Disclosure Statement:
None of the authors declared a conflict of interest
Funding Sources:
No financial support was received for this study.
References
Corresponding Author
Dr.Ali Can Bulut
Department of Prosthodontics, Faculty of Dentistry, University of Kırıkkale, Kırıkkale, Turkey.
Email: alicanbulut @ outlook.com
Table 1. The application of the restorative systems was determined as right upper, left upper, left lower and right lower jaws as follows. The study started from a lesion in the posterior lesion in the right upper jaw of the first patient. The restorative systems were applied to the patients in groups 1 to 6 respectively following the proposals of the manufacturers.
|
Group |
Material |
Type |
|
1. group |
Giomer system (n:50) |
FL-BondII and Beautiful II (FLB&B) |
|
2.group |
Flowable Giomer system (n:50) |
FL-BondII and Beautiful Flow Plus F00 (FLB&BF) |
|
3.group |
Compomer system (n:50) |
Prime Bond NT and Dyract XP (PBNT&DyXP) |
|
4.group |
Flowable Compomer system (n:50) |
Prime Bond NT and Dyract Flowable (PBNT&DyF) |
|
5.group |
Composite system (n:50) |
Single Bond Universal and Filtek Ultimate (SBU&FU) |
|
6.group |
Flowable Composite system (n:50) |
Single Bond Universal and Filtek Ultimate Flow (SBU&FUF) |
*300 NCCLs case in 33 patients (at least 8 in each) regardless of etiology.
Table 2. Products, Lot Numbers, Manufacturer, Composition
|
Product |
Lot Number |
Manufacturer |
Composition |
Filler Content (by volume%) |
|
Beautifil II |
0913 |
Shofu Inc. Kyoto, Japan |
Bis-GMA /TEGDMA resin, multifunctional glass filler and S-PRG (Surface Pre-Reacted Glass-ionomer) filler based on fluroboroalüminosilicate glass, DL-Camphorquinone |
68.6 vol% |
|
Beautifil Flow Plus F00 |
101355 |
|
Bis-GMA /TEGDMA resin, multifunctional glass filler and S-PRG filler based on fluroboroaluminosilicate glass, DL-Camphorquinone |
47vol% |
|
FL- BondII |
031301 |
|
Primer: Carboxylic acid monomer, Phosphonic acid monomer, 6-MHPA, Water, Solvent, Photo-initiator Adhesive: HEMA, UDMA, TEGDMA, 40% fluoride releasing and recharging S-PRG filler, Photo-initiator. |
- |
|
DyractXP |
1402000508 |
Dentsply, Konstanz, Germany |
UDMA, TCB, TEGDMA, TMPTMA, Dimethacrylate resins, Camphorquinone, Ethyl-4 (dimethylamino) benzoate, Butylated hydroxy toluene (BHT), Strontium-alumino-sodium-fluoro-phosphor-silicate glass, Highly dispersed silicon dioxide, Strontium fluoride Iron oxide pigments and titanium oxide pigments, strontium alimino-sodiumfluoro- silicate glass, Strontium fluoride glass particles (0.8 μm) |
50 vol% |
|
Dyract Flow |
1305000624 |
|
Strontium-alimino-fluoro-silicate glass, ammonium salt of PENTA, N, N-dimethyl aminoethyl methacrylate, carboxylic acid modified macromonomers, iron pigments, titanium dioxide |
38vol% |
|
Prime&Bond NT |
1310000536 |
|
Di and trimethacrylate resins, functional amorphous silica, PENTA, cetylamine hydrofluoride, acetone, Photoinitiators, Stabilisers |
- |
|
Filtek Ultimate (Body) |
N625514 |
3M ESPE, St.Paul, MN, ABD |
Bis-GMA, UDMA, TEGDMA, PEGDMA, Bis-EMA, 20 nm silica particuls,4 - 11 nm zirkonyum, particuls |
63.3vol% |
|
Filtek Ultimate Flowable |
N476252 |
|
Bis-GMA, UDMA, Bis-PMA, TEGDMA, Procrylat resins 75 nm Silica nanofiller 15 - 20 nm zirconia nanofiller, ytterbium trifluoride filler |
46 vol% |
|
SingleBond Universal |
494498 |
|
Bis-GMA, HEMA, polyalkenoic acid copolymer, water, ethanol, dimethacrylates |
- |
Table 3. Placement restorations
|
Groups |
Etching Prosedure |
Adehesive |
Restorative Material |
|
FLB&B |
- |
FL- BondII self etching primer was applied to the whole surface of the cavity by using the applicator for 10 seconds and slightly dried five seconds. FL-BondII bonding agent was applied to the whole surface of the cavity by using another applicator and adhesive was light-cured for 5 seconds. |
Beautifil II was placed into the cavity in 2mm layers, and each layer was light cured for 10 seconds. |
|
FLB&BF |
|
|
Beautifil Flow Plus F00 was placed into the cavity in 2mm layers, and each layer was light cured for 10 seconds. |
|
PBNT&DyXP |
3M ESPE Scotchbond universal etchant (3M ESPE, ABD ) was applied for 30 seconds for enamel margins and 15 seconds to dentin surfaces. After etching, the lesion was rinsed for 10 seconds and dried to remove excess water, leaving a moist surface. |
Prime&Bond NT was applied to the whole surface of the cavity with the apllicator and left undisturbed for 20 seconds. The solvent was removed for five seconds with a gentle stream of air and the adhesive was light-cured for 10 seconds |
DyractXP was placed into the cavity in 2mm layers, and each layer was light cured for 20 seconds. |
|
PBNT&DyF |
|
|
Dyract Flow was applied to the lesion incrementally, as mentioned above, and each layer was light cured for 20 seconds. |
|
SBU&FU |
|
SingleBondUniversal was applied to the whole surface of the cavity with the apllicator and left undisturbed for 20-20 seconds. The solvent was removed for five seconds with a gentle stream of air and the adhesive was light-cured for 10 seconds. |
Filtek Ultimate (Body) was placed into the cavity in 2mm layers, and each layer was light cured for 5 seconds. |
|
SBU&FUF |
|
|
Filtek Ultimate Flowable was placed into the cavity in 2mm layers, and each layer was light cured for 5 seconds. |
|
Light polymerized using a Pen-Style LED Curing Light (Elipar S10, 3M ESPE, Germany) |
|||
Table 4. Modified/USPHS Evaluation Criteria and Catagories
|
|
Alpha |
Bravo |
Charlie |
|
Retention |
No loss of restorative material |
- |
Loss of restorative material |
|
Secondary Caries |
No caries present |
- |
Caries present |
|
Anatomic Form |
Continuous |
Discontinuous, no dentin exposed |
Discontinuous, dentin exposed |
|
Surface Texture |
Enamel-like surface |
Surface rougher than enamel, clinically acceptable |
Surface unacceptably rough |
|
Marginal Adaptation |
Closely adapted, no visible crevice |
Visible crevice, explorer will penetrate |
Crevice in which dentin is exposed |
|
Marginal Discoloration |
No discoloration |
Discoloration without axial penetration |
Discoloration with axial penetration |
|
Color Match |
Matches tooth |
Acceptable mismatch |
Unacceptable mismatch |
Table 5. Percent of Survival Rate
|
SURVIVAL RATE (%) |
|||||
|
Groups |
Base Line |
3. Month |
6. Month |
9. Month |
12. Month |
|
FLB&B |
100 |
70 |
68 |
68 |
68 |
|
FLB&BF |
100 |
72 |
70 |
70 |
68 |
|
PBNT&DyXP |
100 |
96 |
88 |
86 |
84 |
|
PBNT&DyF |
100 |
100 |
96 |
96 |
96 |
|
SBU&FU |
100 |
98 |
98 |
98 |
98 |
|
SBU&FUF |
100 |
100 |
100 |
98 |
94 |
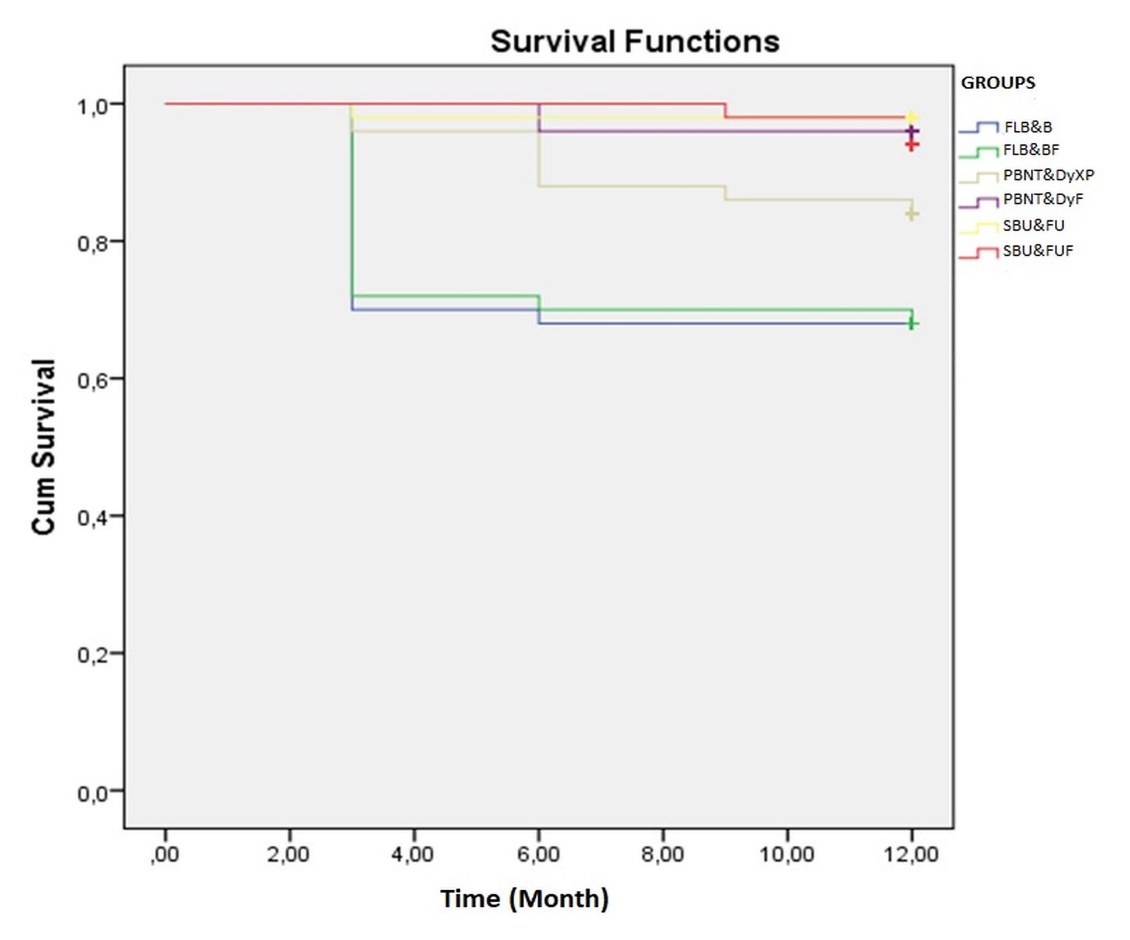
Figure 1. Cumulative survival rates of restorations
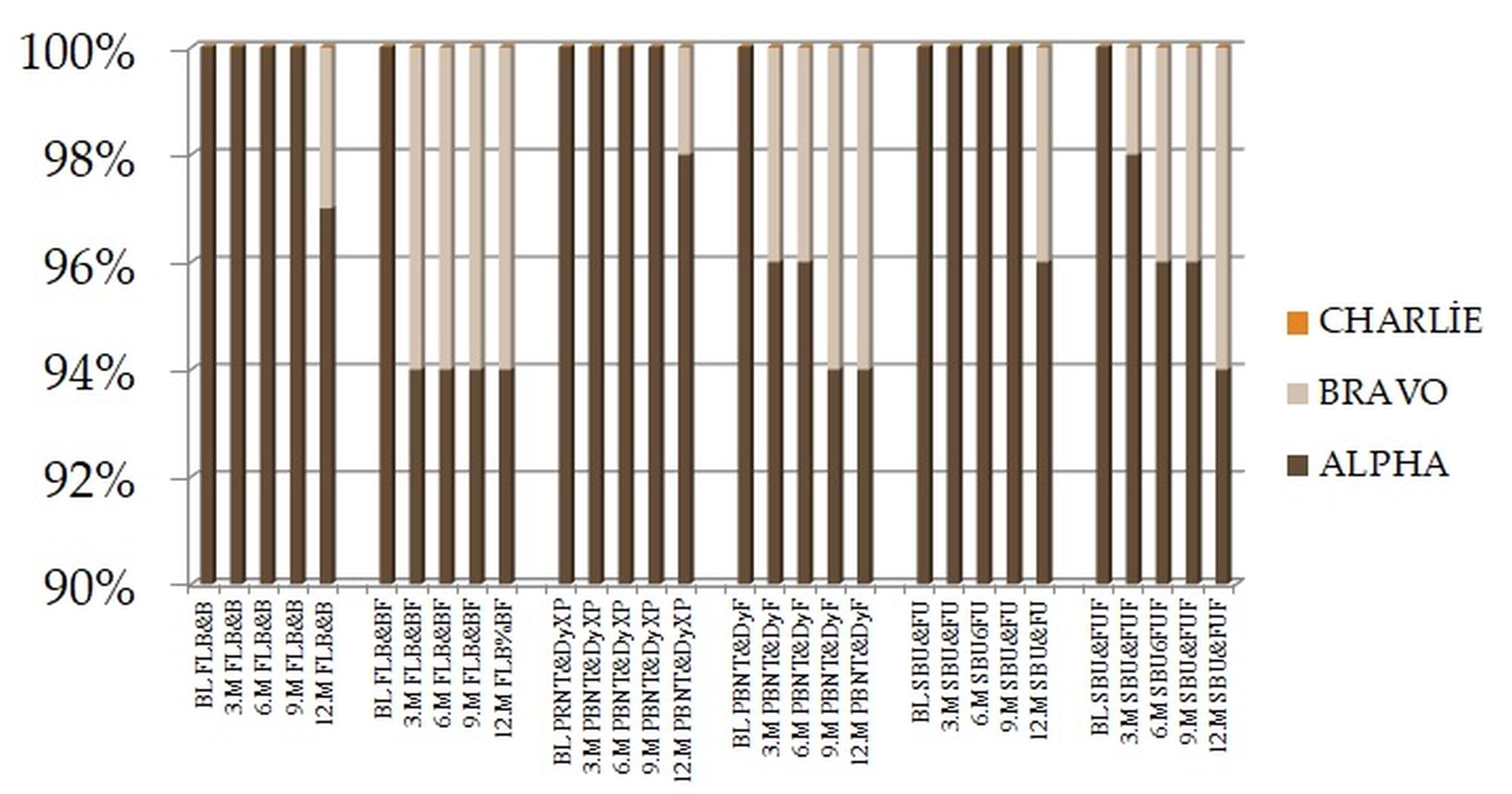
Figure 2: Anatomic Form
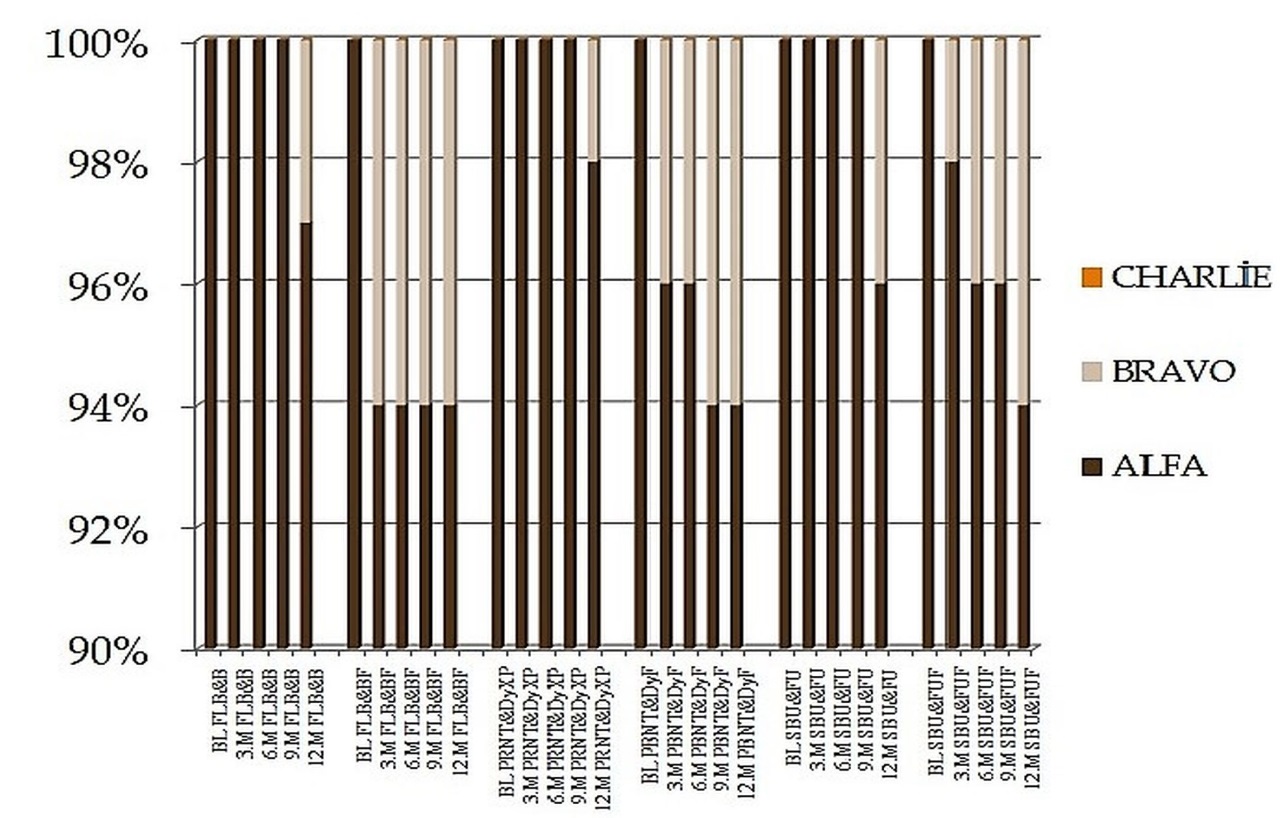
Figure 3: Surface Texture

Figure 4: Color Match

Figure 5: Marginal Discoloration